Our feet carry us through a lifetime, yet they’re often the most neglected part of senior health. As we age, our feet undergo significant changes.
The skin becomes thinner and more fragile, the natural fat pads that cushion our steps gradually diminish, and circulation slows down, making healing more difficult. Joint stiffness increases, and the arch support that once came naturally may weaken.
These changes are simply part of the aging process that requires our thoughtful response.
This guide provides practical steps for keeping your feet strong, comfortable, and healthy right at home. You’ll discover daily care routines, strategies, and guidance on when professional help becomes necessary. Because every step you take toward proper foot care today keeps you active, mobile, and confident tomorrow.

How aging affects your feet
Before diving into care strategies, it’s helpful to understand what’s happening to your feet as the years pass.
Common age-related foot changes include:
- Thinner skin and lost elasticity: Your foot skin becomes more fragile, like tissue paper, making it more vulnerable to tears and injuries.
- Reduced fat padding: The natural cushioning under your heels and the balls of your feet gradually disappears, causing walking on hard surfaces to feel uncomfortable.
- Slower circulation: Blood flow to your feet decreases meaning cuts and wounds that once healed in days may now take a week or longer.
- Weaker muscles and ligaments: Foot strength and flexibility decline over time, potentially flattening your arches and making balance less steady.
- Thicker, brittle toenails: Nails become harder to trim and more prone to fungal infections as you age.
- Changed nerve sensitivity: Many seniors, especially those with diabetes, experience numbness, tingling, or reduced ability to feel pain in their feet.

How to care for aging feet: 12 useful tips
Tip 1: Keep feet clean and dry daily
Wash your feet gently each day with warm, not hot, water and a mild, fragrance-free soap. Hot water can strip away natural oils and dry out your already-vulnerable skin. Take your time, washing between each toe and around the ankles where dirt and sweat accumulate.
Here’s the crucial step many people miss: drying thoroughly, especially between the toes. Moisture trapped between toes creates the environment for fungal infections.
Pat your feet dry with a soft, clean towel, paying special attention to the spaces between each toe. If bending down is difficult, try sitting on a shower chair or placing your foot on a small stool.
Tip 2: Moisturize
Daily moisturizing becomes essential for preventing the painful cracks and fissures that can develop on dry heels and soles. Choose foot creams or lotions containing ingredients like urea (which helps soften thick, hardened skin), shea butter, glycerin, or ceramides.
Apply moisturizer daily, ideally right after washing and drying your feet when your skin is most receptive. Focus particularly on your heels and the soles of your feet, where skin tends to thicken and crack most easily. Never apply lotion between your toes.
Massage the lotion using gentle circular motions. If your feet are extremely dry, consider applying moisturizer before bed and wearing clean cotton socks overnight to lock in moisture.
Tip 3: Inspect your feet every day
Daily foot inspection is perhaps the most important preventive measure in elderly foot care. Small problems caught early stay small; unnoticed issues can escalate into serious complications requiring medical intervention.
Set aside a specific time each day to examine both feet carefully. Look for:
- Cuts, scrapes, or blisters, no matter how small
- Redness, swelling, or warm spots that might indicate infection
- Changes in skin color, including blue or purple toes suggesting circulation problems
- Dry, cracked skin that could become infected
- Changes in toenail appearance, including discoloration, thickness, or separation from the nail bed
- Any changes in sensation, new numbness or tingling

Tip 4: Trim toenails properly and safely
Improper trimming is one of the leading causes of painful ingrown toenails, which can become seriously infected in older adults.
The proper technique:
- Trim your toenails straight across, never rounded or curved down at the edges.
- Use clean, sharp nail clippers specifically designed for toenails (they’re larger and stronger than fingernail clippers).
- Cut the nail even with the tip of your toe, then use an emery board to smooth any rough edges.
- Filing in one direction, rather than sawing back and forth, prevents splitting and damage.
The best time to trim is after bathing when nails are softer and easier to cut. Make sure you have good lighting. If your vision isn’t what it used to be, consider using magnifying glasses or asking for help.
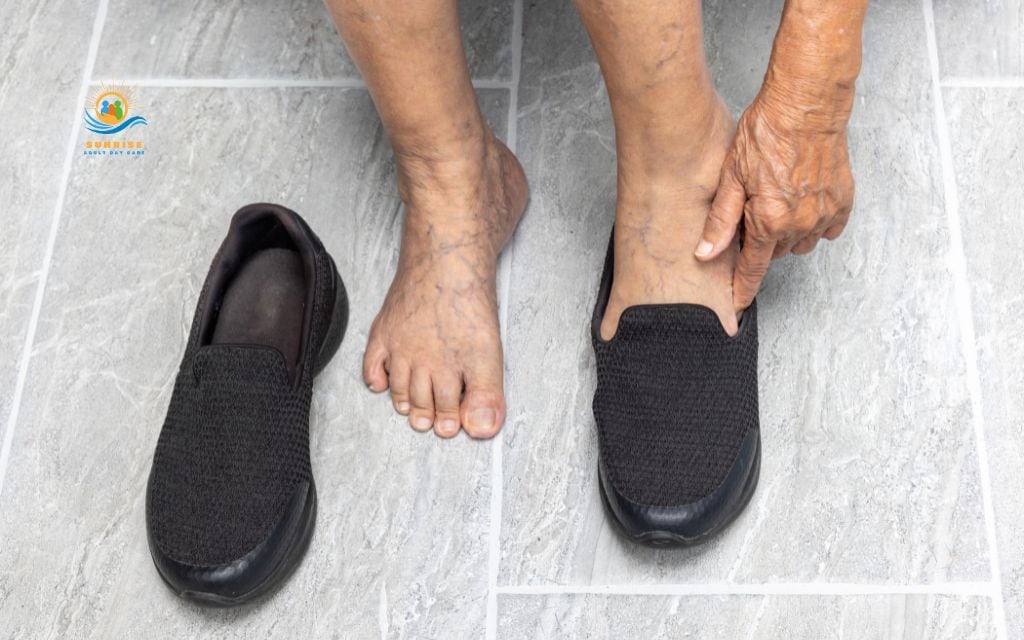
Tip 5: Choose the right footwear
As you age, proper footwear becomes increasingly important for preventing pain, maintaining balance, and protecting your feet from injury.
Look for shoes that offer:
- A wide, roomy toe box that doesn’t squeeze your toes together. Your toes should be able to wiggle freely. Shoes that are too narrow can cause bunions, corns, and hammertoes.
- Firm heel support that cups your heel securely without slipping. The back of the shoe (heel counter) should be sturdy enough to hold its shape when you press on it.
- Non-slip soles with good traction. Look for rubber soles with tread patterns that provide grip.
- Breathable materials like leather or mesh that allow air circulation and reduce sweating. Good ventilation prevents fungal infections and keeps feet more comfortable.
- Adequate cushioning, particularly in the heel and ball of the foot where you’ve lost natural padding.
- Consider shoes with removable insoles so you can add custom orthotics if needed.
Replace worn-out shoes regularly. Old footwear loses support and cushioning, straining your joints and causing pain. If the tread is worn smooth, the heel is leaning to one side, or the insole is compressed flat, it’s time for new shoes.
Tip 6: Wear clean, comfortable socks
Choose socks made from moisture-wicking materials or cotton blends that draw sweat away from your skin. Avoid 100% synthetic fabrics that trap moisture. The right socks reduce friction between your feet and shoes, preventing blisters and calluses.
Avoid socks with tight elastic bands at the top that can restrict blood flow to your feet and lower legs. If you notice deep grooves in your skin when you remove your socks, they’re too tight. Look for socks labeled “non-binding” or “diabetic socks,” which have gentler elastic that won’t constrict circulation.
Change your socks daily, even if they don’t seem dirty. Fresh socks reduce bacteria and fungus buildup that occurs throughout the day. If your feet perspire heavily, consider changing socks midday as well.
Tip 7: Keep blood flow moving
As circulation naturally declines with age, you need to actively support blood flow through gentle daily exercises.
Try these simple movements you can do while sitting:
- Ankle rotations: Lift one foot slightly off the floor and rotate your ankle in slow circles, 10 times clockwise and 10 times counterclockwise. Repeat with the other foot.
- Toe stretches: Spread your toes as wide as possible, hold for five seconds, then curl them under, hold for five seconds. Repeat 10 times.
- Flex-and-point movements: Point your toes away from you, then flex them back toward your shin. This simple movement activates the calf muscles that help pump blood back to your heart.
- Ankle pumps: While sitting, lift your heels off the floor while keeping your toes down, then lift your toes while keeping your heels down.
- Short walks, indoors or outside, are excellent for circulation. Even walking around your home for 5 minutes every hour makes a difference.
Avoid sitting for long periods with your legs crossed, as this restricts blood flow to your lower legs and feet. When sitting for extended periods, elevate your feet slightly on a small stool to encourage drainage and reduce swelling.
For those participating in adult day programs, structured exercise sessions often include chair exercises and walking activities designed to maintain circulation. These supervised activities provide both physical benefits and social engagement.
Tip 8: Maintain a healthy weight
Your feet carry your entire body weight with every step. Extra pounds translate directly into additional stress on feet, ankles, knees, and hips, often leading to pain, joint damage, and mobility limitations. Even modest weight loss can significantly reduce foot pain and improve mobility. A loss of just 10-15 pounds can decrease the load on your feet by 30-60 pounds.

Tip 9: Manage chronic conditions that affect feet
Certain chronic conditions dramatically increase the importance of foot care for seniors.
Diabetes
This condition tops the list of foot health concerns. High blood sugar levels damage both blood vessels and nerves, making feet vulnerable. If you have diabetes:
- Test your blood sugar regularly and follow your doctor’s management plan closely
- Never, ever walk barefoot, even indoors. A tiny cut from a tack or splinter can become a serious problem
- Wear protective footwear always, including cushioned slippers at home
- Inspect your feet daily without fail, checking for any changes
- See a podiatrist at least three to four times per year, or more if your doctor recommends
Arthritis
Joint inflammation causes stiffness, pain, and reduced mobility in feet and ankles. Use well-cushioned shoes with good arch support. Warm foot soaks (not too hot, and not too long) can provide temporary relief from stiffness. Consider exercises specifically designed for arthritic feet, which your physical therapist can demonstrate.
Peripheral vascular disease
Reduced blood flow to the extremities means slower healing and increased risk of serious complications from minor injuries.
Keep your feet protected, avoid temperature extremes, and report any changes in color, temperature, or sensation to your doctor immediately.
Tip 10: Protect feet from temperature extremes
Winter protection
Cold exposure can cause frostbite. Always wear insulated, waterproof boots with good traction when going outside during cold months. Layer with warm wool or thermal socks, but ensure your boots are roomy enough that socks don’t compress your feet.
The combination of cold temperatures and reduced circulation puts older adults at higher risk for cold-related injuries. If your feet become numb from the cold, warm them gradually. Never with hot water or direct heat sources.
Heat hazards
Here’s a crucial warning: avoid direct contact between your feet and heating pads, electric blankets, or hot water bottles.
Reduced sensation means you might not feel burning until serious damage occurs. This is especially dangerous for those with diabetes or neuropathy. If your feet are cold at night, wear warm socks instead of using heat sources.
Test water temperature with your elbow or a thermometer before soaking feet, ensuring it’s comfortably warm but not hot.
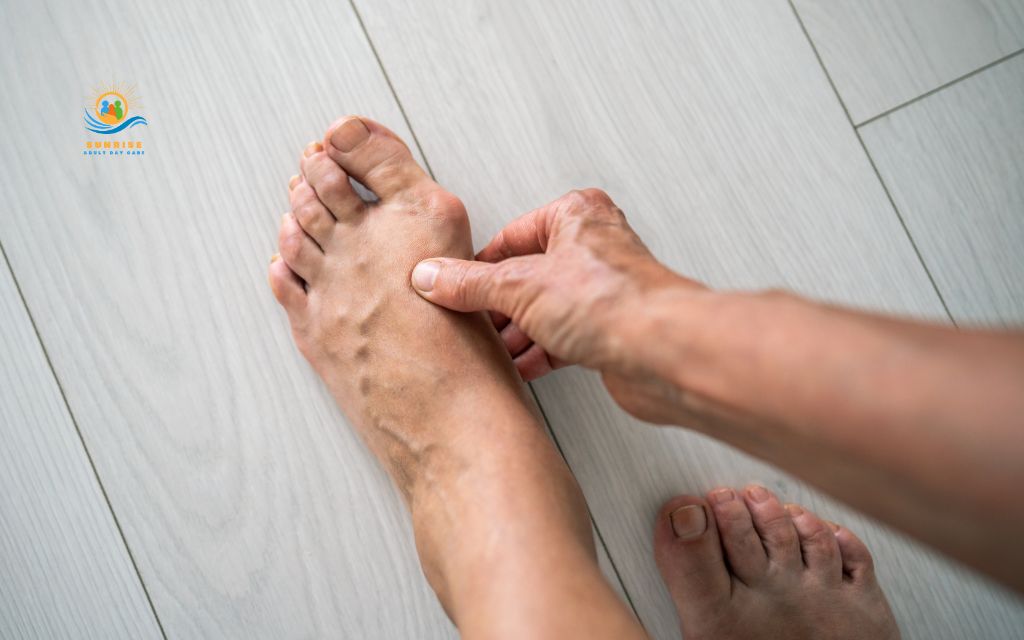
Tip 11: Don’t ignore pain, swelling, or color changes
Pain is your body’s alarm system, and in old people’s feet, it often signals problems that require professional attention. Never adopt a “this is just part of aging” attitude toward persistent foot problems.
Warning signs include:
- Persistent pain that doesn’t improve with rest, ice, and elevation within a day or two.
- Swelling that doesn’t resolve, particularly if it’s only in one foot or if the swollen area feels hot to the touch. These symptoms can indicate infection, blood clots, or circulation problems.
- Color changes are especially concerning. Blue or purple toes suggest circulation problems. Redness with warmth indicates possible infection. Very pale or white skin might signal inadequate blood flow.
- Numbness, tingling, or burning sensations that are new or worsening, particularly if you have diabetes. These symptoms suggest nerve damage.
- Any open sore or wound that doesn’t heal within a few days, or that shows signs of infection (increased redness, pus, red streaks extending from the wound, fever).
Contact your podiatrist, geriatric nurse, or the medical staff at your adult day care center if you notice any concerning changes. Many adult day programs have nursing staff who can provide initial assessment and guide you toward appropriate care.
Tip 12: Schedule regular foot checkups
Preventive care from a qualified podiatrist is just as important as daily home care. Professional foot examinations catch problems early, provide specialized treatments you can’t do at home, and offer personalized guidance for your specific foot health needs.
How often should seniors see a podiatrist?
Most seniors benefit from visits at least once or twice per year. However, if you have diabetes, circulation problems, or mobility challenges that make self-care difficult, you should see a podiatrist 3 to 4 times per year, or as often as your doctor recommends.
Many clinics and adult day centers offer on-site podiatry visits, making professional care more accessible for seniors with transportation challenges.
Conclusion
Healthy feet are the foundation of independence. The 12 tips in this guide aren’t complicated or expensive, but they make a real difference between freely going where you want and being limited by foot pain.
Start with 1 or 2 practices that feel manageable then add more as they become routine. Consistency matters more than perfection. 5 minutes of daily attention to your feet pays tremendous dividends in maintaining mobility and quality of life.
__________
About Sunrise Adult Daycare
At Sunrise Adult Daycare, we provide comprehensive wellness support including health monitoring and access to visiting podiatry services. Our Denver adult day program offers structured exercise programs to maintain circulation and mobility, plus the social engagement that keeps seniors thriving.
For foot care support or wellness information, call (303) 226-6882 to learn about our programs and schedule a visit.
Frequently Asked Questions (FAQs)
How do you take care of your feet as you get older?
Daily elderly foot care includes washing and drying feet (especially between toes), moisturizing heels and soles, inspecting for cuts or changes, trimming toenails, wearing supportive shoes with non-slip soles, changing socks daily, and doing gentle exercises like ankle rotations. See a podiatrist at least once or twice yearly for professional care.
Why do older adults have more foot problems?
Aging causes thinner skin with less fat padding, slower circulation, weaker muscles and ligaments, and thicker toenails prone to fungal infections. Chronic conditions like diabetes, arthritis, and vascular disease compound these changes. Reduced sensation may prevent seniors from noticing injuries early, and slower healing increases infection risk.
What is the best moisturizer for senior feet?
Look for foot creams containing urea (10-20%), shea butter, glycerin, or ceramides. CeraVe, Eucerin, and AmLactin make effective formulations for dry, aging skin. Apply after washing and drying feet, focusing on heels and soles. Avoid applying between toes, and choose fragrance-free products for sensitive skin.
How should elderly toenails be trimmed safely?
Trim toenails straight across using clean toenail clippers, never rounded. Cut even with the toe tip, then smooth edges with an emery board. Trim after bathing when nails are softer, with good lighting. If nails are thick, brittle, or difficult to cut, see a podiatrist.
How often should seniors see a podiatrist?
Most seniors should visit a podiatrist 1 or 2 yearly. Those with diabetes need 3 to 4 visits annually or more as recommended. Seniors with circulation problems, mobility limitations, or chronic foot issues may need more frequent care. Schedule appointments immediately for persistent pain, swelling, color changes, or wounds that don’t heal.





