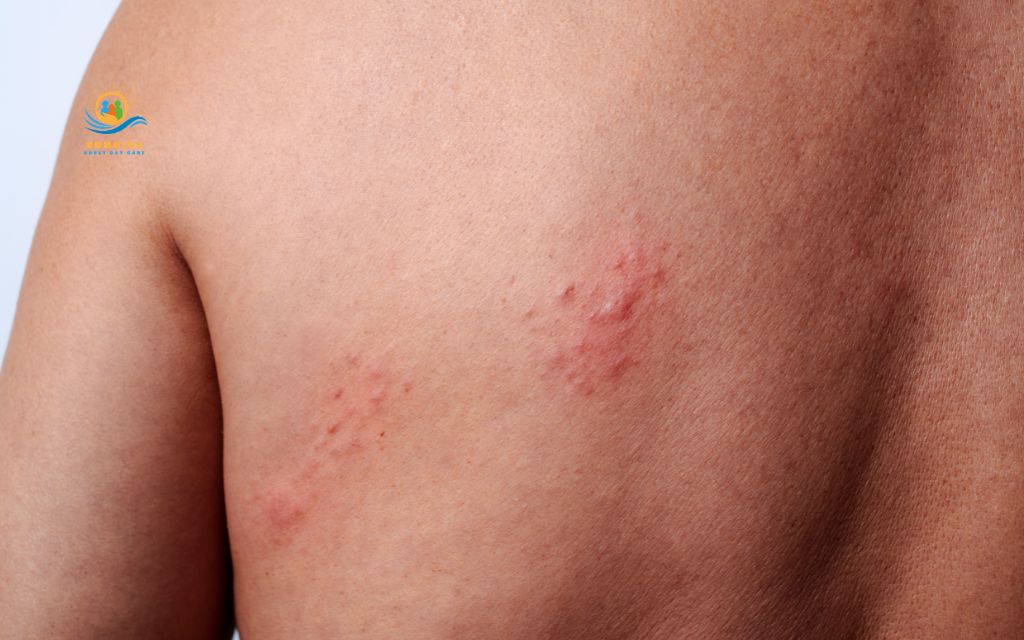
If you or someone you love attends an adult day care program, a shingles outbreak raises immediate questions: Is this shingles? Should I call the doctor today? Can I still come to the program? This guide gives you clear, medically accurate answers, so you can act fast, stay safe, and recover with confidence.
What is shingles?
Shingles (herpes zoster) is a painful skin rash caused by the reactivation of the varicella-zoster virus – the same virus responsible for chickenpox.
After a person recovers from chickenpox, the virus does not disappear. Instead, it retreats silently into nerve tissue near the spinal cord and brain, where it can remain dormant for decades.
For most people, the immune system keeps the virus suppressed indefinitely. But in older adults, that protection can weaken, and when it does, the virus can reactivate and travel along nerve pathways to the skin, producing the distinctive rash and burning pain that characterize shingles in old people.
Why does this matter more with age?
- The risk of shingles increases sharply after age 50 and rises again after age 60.
- Pain tends to be more severe in older individuals.
- The risk of long-term nerve pain is significantly higher in seniors than in younger adults.
- Shingles in elderly people with weakened immune systems from chronic conditions such as diabetes, heart disease, or cancer can be more difficult to treat and slower to heal.
The single most important fact to remember: Antiviral treatment started within 72 hours of rash or symptom onset significantly reduces severity, duration, and the risk of PHN. Every hour counts.
What causes shingles in old people?
Understanding the cause helps older adults and their families recognize risk factors and take prevention seriously.
The biology of reactivation
The varicella-zoster virus belongs to the herpesvirus family. After a primary chickenpox infection – which most adults over 50 experienced in childhood – the virus travels up sensory nerves and establishes a permanent, dormant residence in the dorsal root ganglia (nerve clusters near the spine) or the trigeminal ganglia (near the face and head).
For decades, the immune system – specifically T-cell immunity – suppresses viral replication. When that immune control weakens, the virus can reactivate, replicate, and migrate down the nerve toward the skin.
Why shingles and old age go together
Several age-related changes increase vulnerability:
- Immune senescence: The natural decline of the immune system that comes with aging reduces the body’s ability to keep the dormant virus suppressed.
- Chronic illness: Conditions common among older adults, including diabetes, COPD, and autoimmune disorders, further impair immune function.
- Medications: Immunosuppressive drugs used for conditions like rheumatoid arthritis or organ transplantation increase reactivation risk.
- Physical or emotional stress: Illness, surgery, grief, or even a demanding schedule can temporarily suppress immune function enough to trigger reactivation.
The relationship between shingles and old age is well established: approximately half of all shingles cases occur in adults over age 60. Understanding this connection empowers seniors and caregivers to recognize symptoms early and act without delay.
Early signs of shingles in old people: Recognize it before the rash
One of the most important facts about shingles in old people is that the rash is not the first symptom. There is typically a pre-rash phase lasting one to five days during which early warning signs appear. Recognizing these signs before the blisters form gives you the best possible window for effective antiviral treatment.
Stage 1: Pre-rash symptoms (days 1–5)
The following symptoms may appear on one side of the body, usually the torso, face, or neck, in the days before any visible rash:
- Burning, tingling, or stabbing pain along a specific band or strip of skin
- Unusual skin sensitivity, even light touch from clothing may feel uncomfortable
- Itching or numbness in the affected area
- Mild flu-like symptoms, including low-grade fever, fatigue, headache, or sensitivity to light
Many people initially mistake these sensations for a pulled muscle, a pinched nerve, or a dental problem (when the face is involved). In older adults especially, this pre-rash pain can be quite intense before any visible sign appears.
If you or a loved one experiences one-sided burning or skin pain without an obvious cause, contact a healthcare provider right away. Do not wait for a rash to appear before calling.
Stage 2: The rash phase
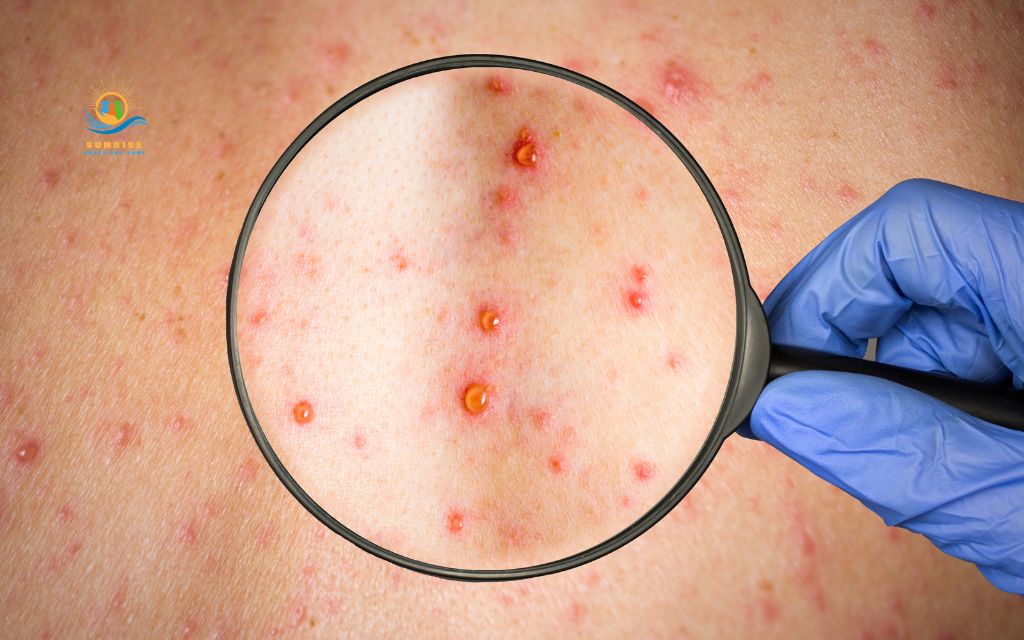
Within a few days of the prodromal symptoms, the rash appears:
- Red, inflamed patches develop along the affected nerve pathway (dermatome)
- Fluid-filled blisters form on top of the red patches within 24 – 48 hours
- The rash follows a band-like or stripe pattern on one side of the body, most commonly wrapping around the torso from the spine to the chest or abdomen
- Facial involvement is possible, particularly around the forehead, eye, or ear
Shingles almost always affects only one side of the body. A rash that crosses the midline or appears symmetrically is unlikely to be shingles.
Over 7 to 10 days, the blisters fill, rupture, and begin to crust over. Once all lesions have fully crusted, the person is no longer contagious through direct contact.
Why shingles is dangerous for seniors
Shingles in elderly people is not simply an uncomfortable rash. Without prompt treatment, it can lead to serious, sometimes permanent complications.
Understanding the risks helps older adults and caregivers prioritize speed of treatment.
Postherpetic neuralgia (PHN)
Postherpetic neuralgia is the persistence of nerve pain after the shingles rash has completely healed. It occurs because the virus causes lasting damage to pain-transmitting nerve fibers.
- PHN affects approximately 10–18% of all shingles patients, but the rate rises substantially after age 60.
- Pain can range from a constant dull ache to severe, debilitating burning or electric-shock sensations.
- PHN can last months and in some cases, years.
- Everyday activities including dressing, bathing, and sleeping can become deeply painful.
- Depression, anxiety, and social withdrawal are common secondary effects of long-term PHN in older adults.
Starting antiviral medication within 72 hours significantly lowers the risk of developing PHN. This is the most compelling reason for urgent medical attention at the first sign of shingles in old age.

Ophthalmic shingles
When shingles affects the ophthalmic branch of the trigeminal nerve – a condition called herpes zoster ophthalmicus – the rash appears on the forehead, eyelid, or tip of the nose. This is a medical emergency.
Complications can include:
- Keratitis (corneal inflammation) potentially causing scarring and vision loss
- Uveitis (internal eye inflammation)
- Increased risk of glaucoma and other chronic eye conditions
If there is any rash near the eye – including on the forehead above the eye or on the tip of the nose – seek emergency care or an urgent ophthalmology evaluation the same day.
Other serious complications
| Complication | Description |
| Ramsay Hunt syndrome | Shingles affecting the facial nerve; causes ear pain, facial weakness, and hearing loss |
| Bacterial superinfection | Open blisters can become infected with bacteria, leading to cellulitis or abscess |
| Hospitalization | Severe or complicated cases – particularly in frail or immunocompromised seniors – may require inpatient care |
| Stroke risk | Some research suggests shingles – particularly ophthalmic shingles – may modestly increase short-term stroke risk in older adults |
| Increased frailty | Recovery from shingles can accelerate functional decline in already vulnerable seniors |
What to do today: Your action plan for the first 72 hours
If you suspect shingles, even before a rash appears, here is what to do immediately.
Step 1: Call your healthcare provider right now
Do not wait to see if symptoms worsen. Do not wait for the rash to fully develop. Call your primary care provider, urgent care clinic, or a nurse line today and describe:
- The location and nature of the pain or skin sensation
- Whether any rash or blisters have appeared
- Your age and any underlying health conditions or immunosuppressive medications
Most providers can diagnose shingles clinically – based on your description of symptoms and the location of the rash – without waiting for lab confirmation. Time is the deciding factor for treatment effectiveness.
Step 2: Ask about antiviral medication
Three antiviral medications are currently approved for treating shingles:
- Valacyclovir (Valtrex): the most commonly prescribed option for older adults
- Acyclovir (Zovirax): an older option
- Famciclovir (Famvir): another oral option
These medications work by suppressing viral replication. When started within 72 hours of rash onset, they:
- Reduce the severity and duration of the acute rash
- Decrease pain during the active phase
- Significantly lower the risk of postherpetic neuralgia
- May reduce the risk of complications such as ophthalmic involvement
After 72 hours, antivirals are less effective but your provider may still prescribe them if new blisters are still forming or if you have risk factors for complications.
Step 3: Manage pain safely
Shingles pain in older adults can be significant. Work with your healthcare provider to find a safe, appropriate pain management approach. Options may include:
- Over-the-counter pain relievers such as acetaminophen (Tylenol) or ibuprofen for mild-to-moderate pain (check with your provider if you have kidney or liver concerns)
- Prescription medications including gabapentin, pregabalin, or tricyclic antidepressants – these are especially useful for nerve pain
- Topical treatments such as lidocaine patches or capsaicin cream applied to the affected area once blisters have crusted
- Cool, moist compresses applied gently to the rash area to soothe irritation
- Loose, soft clothing that minimizes friction against sensitive skin
- Calamine lotion to reduce itching and provide mild topical relief
Avoid scratching blisters. This increases the risk of bacterial infection and scarring.
Is shingles contagious in adult day care and group settings?
This is one of the most important practical questions for seniors who attend adult day care programs and for the staff and families supporting them.
How shingles spreads (and how it doesn’t)
Shingles itself is not airborne and not spread through casual contact like a cold or flu. However, the varicella-zoster virus can be transmitted from an active shingles rash to a person who has never had chickenpox or the chickenpox vaccine and in that unvaccinated person, it would cause chickenpox, not shingles.
Transmission requires direct contact with fluid from open blisters.
Key facts:
- The virus cannot spread before the rash appears. The pre-rash pain phase is not contagious.
- Once all blisters have crusted over (typically 7–10 days after rash onset), the person is no longer contagious.
- A covered rash that is not oozing presents minimal risk in group settings, provided good hygiene is maintained.
Who is at risk in a group setting?
In an adult day care program, certain participants face higher risk from exposure:
- Unvaccinated individuals who have never had chickenpox
- Immunocompromised individuals, including those on chemotherapy, high-dose steroids, or with HIV
- Pregnant women (including younger staff members)
- Newborns or very young infants who may be brought to the program by visiting family

Red flags: When to seek urgent or emergency care
Most cases of shingles in older people can be managed with outpatient treatment. However, certain symptoms require same-day urgent attention or emergency care.
Do not wait – call your provider or 911 immediately if you notice any of the following:
- Rash on or near the eye – forehead above the brow, eyelid, or tip of the nose
- Severe or worsening headache that is different from usual headaches
- Confusion, disorientation, or altered mental status could signal viral encephalitis
- High fever
- Weakness or paralysis on one side of the face or body
- Hearing loss or severe ear pain with rash near the ear
- Rash spreading rapidly beyond one side of the body
These symptoms, while uncommon, can signal serious neurological or ocular involvement that requires immediate specialist intervention.
How adult day care programs support seniors with shingles
At Sunrise Adult Daycare, we understand that a shingles diagnosis affects not just physical health, but emotional well-being and social connection as well.
Our approach is built around dignified, compassionate, and evidence-informed support throughout the recovery process.
Symptom monitoring and coordination
Our trained staff are attentive to signs of illness among participants, including early indicators of shingles such as unexplained one-sided pain, skin sensitivity, or unusual fatigue. When staff observe or a participant reports potential symptoms, we:
- Encourage immediate contact with the participant’s healthcare provider
- Notify family caregivers or emergency contacts
- Provide medication reminders for antivirals and pain management as directed by the treating clinician
Infection control protocols
Protecting all participants, especially those who may be immunocompromised or unvaccinated, is a core part of our safety commitment.
Our infection control procedures for shingles include:
- Verifying that any returning participant with a shingles history has fully crusted lesions, covered rash, and provider clearance
- Reinforcing hand hygiene practices among staff and participants
- Ensuring linens, seating surfaces, and shared equipment are regularly sanitized
- Educating staff on identifying high-risk contacts who should be notified in the event of a possible exposure
Comfort, engagement, and emotional support
Recovering from shingles can be isolating and discouraging. We support participants through:
- Modified activity programming during recovery that accommodates reduced energy or physical limitations
- Gentle engagement options such as quiet social activities, music appreciation, and light cognitive games
- Emotional reassurance from staff who understand the challenges of shingles in older people and can provide a warm, patient, judgment-free environment
- Connection with peer participants to reduce the isolation that often accompanies a painful illness
- Coordination with family members to ensure continuity of care between the daycare setting and the home
If your loved one is recovering from shingles or you have questions about our infection control policies and our daycare program, contact Sunrise Adult Daycare at 303-226-6882.
Conclusion
Shingles in seniors is common but it is not something to accept passively. With the right response at the right time, most older adults can recover fully and minimize their risk of lasting complications.
Here is your clear, three-part action plan:
- Act within 72 hours. At the first sign of shingles, call your healthcare provider and ask about antiviral medication. Speed is everything.
- Manage safely in group settings. Stay home from adult day care until blisters are fully crusted, the rash is covered, and a clinician has confirmed you are no longer contagious. Once those conditions are met, return confidently.
- Protect yourself long-term. Get vaccinated. Even if you’ve had shingles before, vaccination significantly reduces your risk of a future outbreak and PHN.
Shingles does not have to mean weeks of severe pain, months of nerve damage, or withdrawal from the social life and programs that make each day meaningful.
With early treatment, clear return-to-care guidelines, and the protection of an effective vaccine, older adults can face shingles with knowledge, speed, and confidence.
Frequently asked questions (FAQs)
Is shingles dangerous to elderly people?
Yes, shingles can be more serious in older adults. They have a higher risk of long-term nerve pain (postherpetic neuralgia) and complications like eye involvement. Early treatment helps reduce these risks.
How fast should seniors seek treatment?
Seniors should contact a doctor as soon as shingles is suspected. Antiviral medication works best when started within 72 hours of rash or pain onset. Acting quickly can shorten illness and lower complication risk.
Can shingles spread in adult day care?
Yes, shingles can spread through direct contact with fluid from open blisters. It is contagious until the rash has crusted over. Keeping the rash covered reduces transmission risk.
What are the long-term effects of shingles in elderly?
The most common long-term effect is postherpetic neuralgia (PHN), which causes persistent nerve pain. This pain can last months or even years. It is more common after age 60.
Should seniors get the Shingrix vaccine?
Yes, adults aged 50 and older are strongly recommended to receive two doses of Shingrix. The vaccine significantly reduces the risk of shingles and long-term complications. Even those who previously had shingles should get vaccinated.